Sekbio Recombinant Monkeypox Virus Proteins
The World Health Organization has confirmed about 92 monkeypox cases and 28 suspected cases as of May 20. And the pandemic has recently been reported in 12 countries where the disease is not typically detected. "WHO is working with affected and other countries to expand disease surveillance, identify and support those who may be affected, and guide how to manage the disease, " according to a Friday statement.
What is monkeypox?
Monkeypox is a zoonotic viral disease caused by the monkeypox virus, which can be transmitted from animals to humans and from person to person. Monkeypox was first identified in a monkey colony used for research in 1958 and detected in humans until 1970. Monkeypox is general in the rainforests of Central and West Africa, where animals may carry the virus live. Before this pandemic, monkeypox was only endemic in countries such as Central and West Africa. Monkeypox patients were occasionally found in non-mainly endemic areas but generally those traveling to monkeypox-endemic regions.
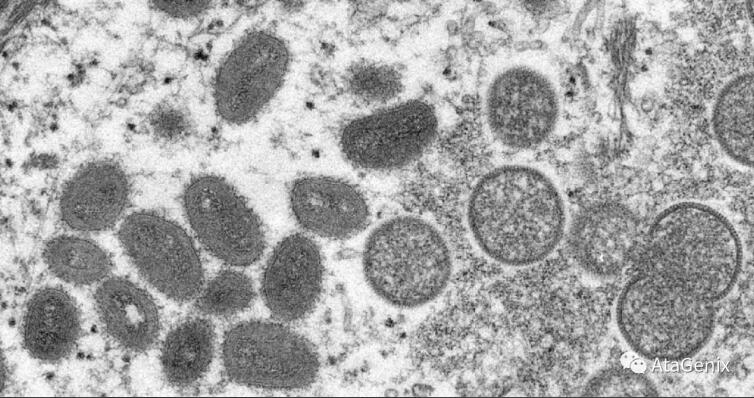
Fig 1. Electron microscope images provided by the CDC in 2003 showed mature oval monkeypox virions (left) and spherical immature virions (right) from human skin associated with the 2003 woodchuck endemic sample.
Three research teams from Portugal, Belgium, and the United States recently published the preliminary sequencing results of the viral genome sequences carried by monkeypox-infected patients on the Virological and NCBI websites. The three gene sequences were obtained from the monkeypox virus carried by a Portuguese patient, a Belgian patient, and a Massachusetts patient, most related to the monkeypox virus that spreads from Nigeria to the UK, Singapore, and Israel. This strain leads to less severe disease and lower mortality than Central Africa's strains.
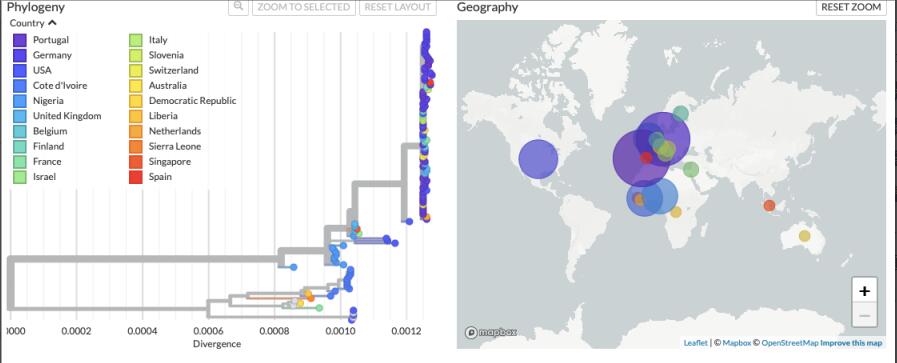
Fig 2. The latest global monkeypox virus genome sampling
Monkeypox is caused by a DNA virus distinct from SARS-CoV-2, a rapidly evolving RNA virus currently circulating worldwide. The monkeypox virus has a more complex structure than SARS-CoV-2, and DNA viruses are more powerful in detecting and repairing mutations than RNA viruses. It means that a rapid mutating to own a strong ability of human-to-human transmission is less likely to occur in monkeypox viruses. But epidemics in non-primary endemic areas and reports of unrelated cases are simultaneously occurring, which deeply worried scientists such as Andrea McCollum, who heads the poxvirus team at the US Centers for Disease Control and Prevention (CDC). It suggests that there may be hidden chains of transmission for the virus.
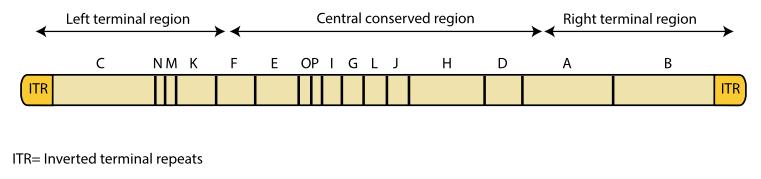
The poxvirus genome is about 200kb and encodes about 200 proteins. It is a linear double-stranded DNA genome with covalently closed hairpin ends (no free 3' or 5' ends). It contains 10kb inverted terminal repeats (ITR) at each end. Genes are closely packed: intergenic regions of more than 100bp are rare.
The central conserved region encodes "housekeeping" genes involved in transcription, replication, and virion assembly. The genes encoded in the terminal areas vary between poxviruses and encode proteins involved in the host range and pathogenesis.
Monkeypox virus has the typical form of orthopoxvirus. The shape is rounded brick or oval, and the size is 200~400nm. The outer layer is a lipoprotein membrane or envelope, and there are two protein-containing lateral bodies in the middle, one thick Membrane core, which contains a large double-stranded DNA gene body. The monkeypox virus genome is double-stranded DNA, about 197 kb in length. It contains an identical but opposite inverted terminal repeat at the end of the genome, and the virus has 190 open reading frames, four located in inverted terminal repeats.
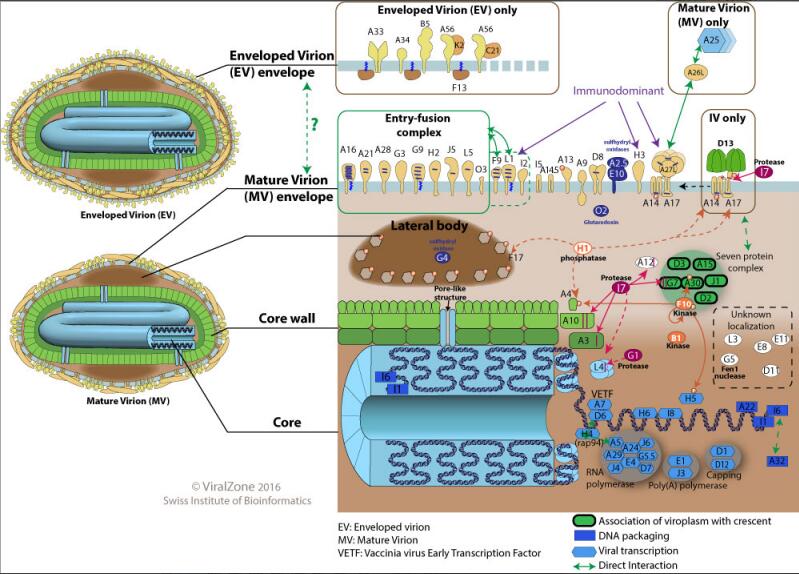
Fig 4. Schematic diagram of poxvirus structural proteins
Symptoms of monkeypox infection
Monkeypox is a self-limiting disease, and the main symptoms generally include fever, severe headache, muscle aches, back pain, lack of energy, swollen lymph nodes, and rash or skin lesions. Lymph gland symptoms are a distinguishing feature of monkeypox. The symptoms usually last two to four weeks and recovery without treatment in most cases. But these symptoms can lead to complications and even death for some people. Newborns, children, and people with underlying immune deficiencies may risk more severe symptoms and death from monkeypox. Complications in severe monkeypox cases include skin infections, pneumonia, confusion, and eye infections that can lead to vision loss. About 3-6% of patients currently reported in endemic countries result in death.
Main epidemic areas and transmission routes in the world
As of May 21, 2022, the World Health Organization (WHO) has received 92 laboratory-confirmed cases and 28 suspected cases reported from 12 countries and regions, including the United Kingdom, the United States, Portugal, Spain, Italy, and Sweden. Based on previous studies, monkeypox is generally considered less contagious because the disease requires close physical contact (e.g., skin-to-skin) with an infectious person to spread from person to person, and the risk to the public is low. Therefore, this round of monkeypox epidemics with rapid global spread and unusual transmission paths is rare. Raising awareness of this new situation will help stop further spread.
People with monkeypox are contagious when they develop symptoms (usually lasting two to four weeks). Rashes, bodily fluids (such as fluid, pus, or blood from skin lesions), and dry scabs are particularly contagious. Sores, lesions, or canker sores in the mouth can also be contagious, which means the virus can spread through saliva. Therefore, people who have close interactions with infectious individuals, including health workers, family members, and sexual partners, are at greater risk. The virus can also be passed through the placenta from a pregnant woman to a fetus. Or from an infected parent to a child through skin-to-skin contact during or after birth. Children are often more prone to severe symptoms than teenagers and adults. It is not known whether asymptomatic patients can spread the disease.
How should we respond to monkeypox?
Monkeypox is a self-limiting disease that generally recovers without treatment. For severe cases, vaccinia immunoglobulin (VIG) is recommended. Both monkeypox and smallpox are orthopoxviruses, so several vaccines against smallpox may provide some protection against monkeypox. A new vaccine developed for smallpox (MVA-BN, also known as Imvamune, Imvanex, or Jynneos) was approved in 2019 to prevent monkeypox, but it is not yet widely available. People vaccinated against smallpox in the past also have some resistance to monkeypox. However, due to the extinction of smallpox in 1980, China stopped large-scale smallpox vaccination in 1981. But some laboratory staff or health workers may have been vaccinated with a newer smallpox vaccine. In January 2022, an antiviral drug used to treat smallpox (tecovirimat, product name TPOXX) was also approved for monkeypox.
The public's attention to the epidemic is gradually rising since the SARS-CoV-2 pandemic. Like humans ultimately defeated smallpox in 1980, it is promising to believe that the progress of modern life science and technology can prevent and cure all kinds of diseases we encounter. After the monkeypox epidemic, research in various directions, including vaccines, drugs, diagnostic reagents, and animal models, has been conducted worldwide.
Sekbio Monkeypox-related products
Product Name | Catalog No. | Target Names | Price(USD/mg) |
Recombinant Monkeypox Virus Protein (A29L) | MVPA29L | A29L | 466 |
Recombinant Monkeypox Virus Protein (A35R) | MVPA35R | A35R | 466 |
Recombinant Monkeypox Virus Protein (M1R) | MVPM1R | M1R | 466 |
Recombinant Monkeypox Virus Protein (A29L)
Gene: A29L
UniProtKB - Q9YN60
10 20 30 40 50
MDGTLFPGDD DLAIPATEFF STKAAKNPET KREAIVKAYG DDNEETLKQR
60 70 80 90 100
LTNLEKKITN ITTKFEQIEK CCKHNDEVLF RLENHAETLR AAMISLAKKI
110
DVQTGRRPYE

















