The Difference between Troponin I (TnI) and Troponin T (TnT)
Cardiac troponin (cTn) is a specific biomarker for myocardial cell injury, garnering increasing attention from clinicians in recent years due to its higher sensitivity and specificity in diagnosing acute myocardial infarction (AMI). But how much do we really understand about this important marker? Let's delve into the world of cardiac troponin together.
Introduction to Troponin
Troponin is a regulatory protein for striated muscle contraction, serving as a structural protein in both skeletal and cardiac muscle. In 1971, troponin was first isolated into troponin I (TnI), troponin T (TnT), and troponin C (TnC). Among them, the cardiac isoforms of troponin T and I possess unique antigenic epitopes, resulting in higher cardiac specificity.
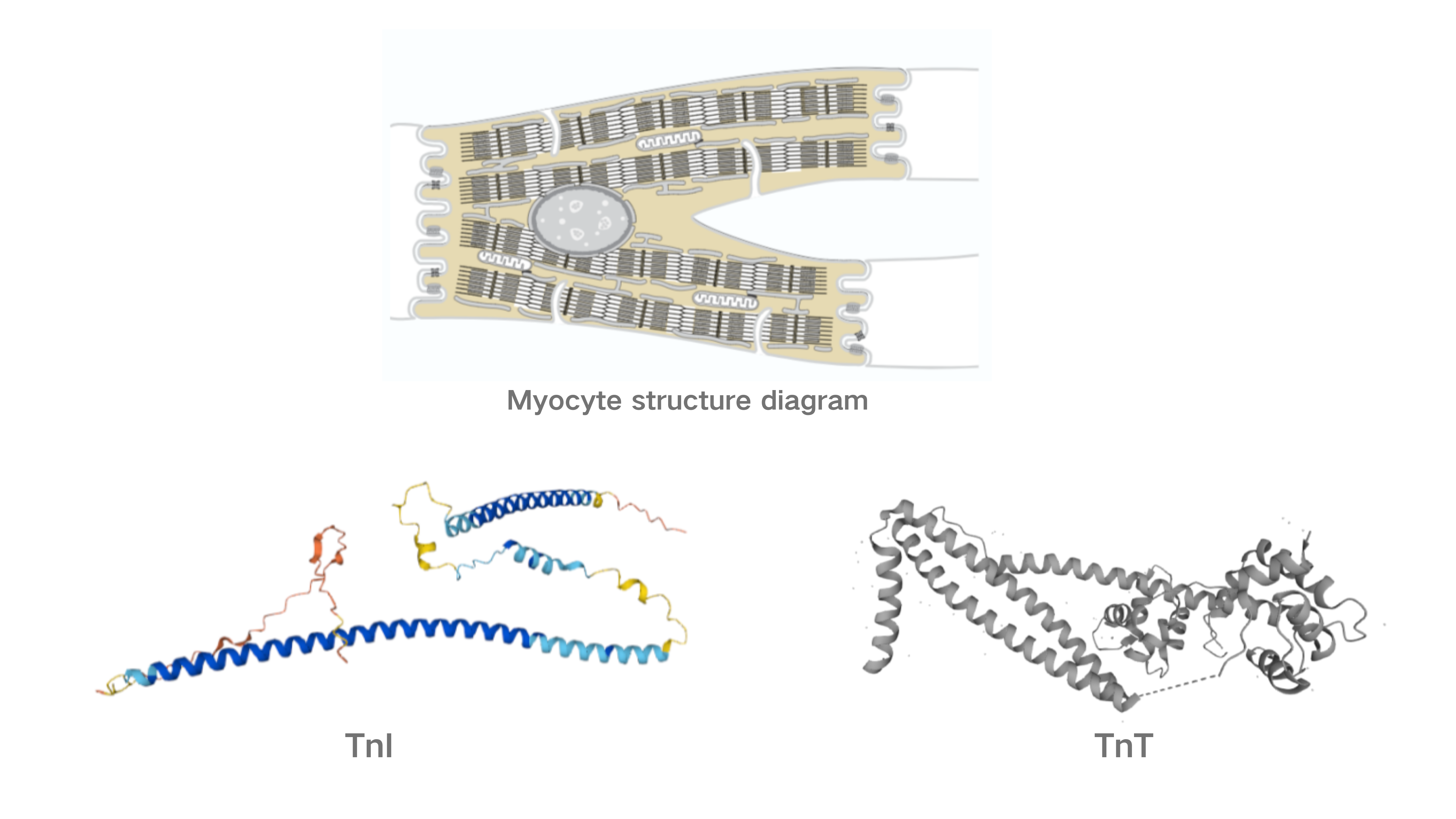
Distinguishing TnT and TnC
During myocardial injury, various forms of cTn may be released. When myocardial cells undergo necrosis, the plasma mainly exhibits free cTnT and cTnI-cTnC complexes.
cTnI and cTnT are widely present in patients' myocardium, and there is a strong correlation between cTnI and cTnT. Their combined application in the diagnosis of heart disease patients can play a complementary role, providing a more comprehensive reference basis for diagnosing patients' diseases.
In recent years, with continuous improvements in detection methods, high-sensitivity cardiac troponin has been widely applied. High-sensitivity cTn aids in detecting previously overlooked minor myocardial injuries, facilitating earlier diagnosis of AMI, more rational screening of high-risk patients for cardiovascular events, and optimizing clinical treatment decisions and prognosis assessment. Below, we mainly enumerate the differences in the clinical application of high-sensitivity cardiac troponin T and high-sensitivity cardiac troponin I.
(1) Time Window: The detection time window of hs-cTnT may be wider than hs-cTnI.
A study on biomarker dynamics showed that hs-cTnT peaked at 11.8 hours in STEMI, followed by a biphasic curve, reaching a second peak at 76.9 hours. In contrast, hs-cTnI peaked at 11.8 hours in STEMI, followed by a linear decline.
(2) Diagnostic Accuracy: Early monitoring of hs-cTnI for NSTEMI may be higher than hs-cTnT.
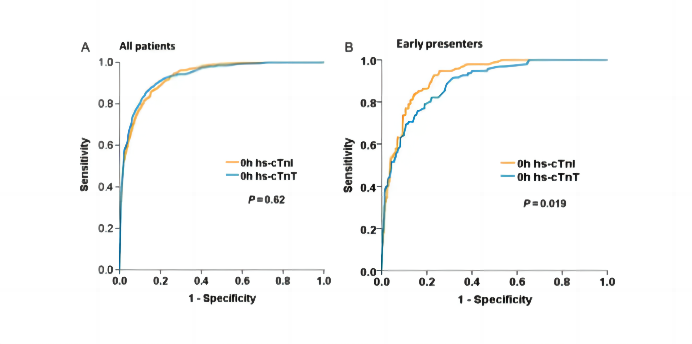
In a prospective study aimed at comparing the accuracy of hs-cTnI and hs-cTnT in the early diagnosis and prognosis prediction of non-ST-segment elevation myocardial infarction (NSTEMI), a total of 2,226 patients presenting with acute chest pain to the emergency department were included, with 18% ultimately diagnosed with NSTEMI. Quantitative analysis of the AUC for NSTEMI subjects showed similar diagnostic accuracy for hs-cTnI and hs-cTnT (P=0.62, Figure A). As shown in Figure B, compared to hs-cTnT, in patients experiencing chest pain within 3 hours (25% of the entire cohort), hs-cTnI significantly improved the diagnostic accuracy for NSTEMI (P=0.019). However, in patients with chest pain lasting more than 3 hours, hs-cTnT demonstrated higher diagnostic accuracy for NSTEMI (P=0.007).
(3) Prediction of Mortality: hs-cTnT may be superior to hs-cTnI in predicting all-cause mortality in emergency patients.
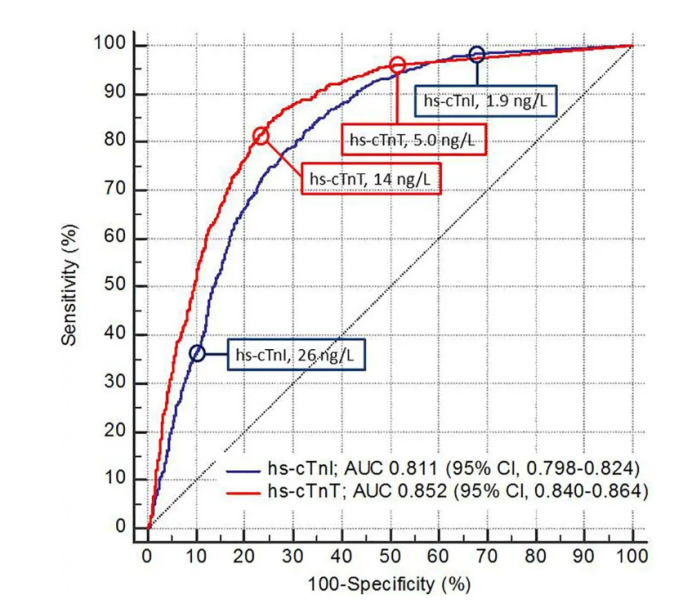
The LITROP study included a total of 3,588 emergency department patients. The results showed that for predicting all-cause mortality, the AUC was 0.811 (95% CI, 0.798-0.824) for hs-cTnI and 0.852 (95% CI, 0.840-0.864) for hs-cTnT. ROC curve comparison revealed that the AUC of hs-cTnT was higher than hs-cTnI, with a difference of 0.041 (p <0.001).
As illustrated in the figures, in predicting all-cause mortality in emergency patients, hs-cTnT was significantly better than hs-cTnI in this study.
(4) Long-term Prognostic Capability: hs-cTnT may be superior to hs-cTnI in predicting long-term prognosis of NSTE-ACS patients.
A related study compared hs-cTnT and hs-cTnI in predicting significant coronary artery damage and long-term prognosis in ACS patients. A total of 390 NSTE-ACS patients were finally included. The study found that hs-cTnT was superior to hs-cTnI in predicting the long-term prognosis of NSTE-ACS patients.
Conclusion
Both cardiac troponin T (cTnT) and cardiac troponin I (cTnI) are widely present in patients' myocardium, providing a basis for the diagnosis of patients' diseases with high specificity, sensitivity, and accuracy. They play a positive role in patients receiving timely and effective treatment and improving prognosis, and have been widely accepted by clinical laboratory workers. Comparing the differences between cTnI and cTnT is of great significance for further improving the clinical application of hs-cTn in the management of suspected AMI patients.

















